Abstract
A ten-year-old reconstruction surgery of a total nasal dorsum defect on the right nose involves a medial arm flap and self-rib cartilage, complicated into fibrous tissue retraction, which caused nostril narrowing and asymmetry. This complication was corrected using a combination of a nasolabial flap for a skin coverage and a modified, old rib cartilage graft to create a supportive rim for the newly reconstructive right nasal ala. There is controversy about the advantage of auricular cartilage versus costal cartilage with a gap in academic studies. However, in this case, costal cartilage has shown significant benefits that helped patients to gain the best functional and aesthetic results. In addition, the modification of an old nasal graft for another function is a unique spotlight in our case. Therefore, we report a case about using an old nasal graft for an alternative function, as well as the observed results from the first-stage of this procedure.
Introduction
The nasal area is the most valuable region on the face, and its reconstruction is often challenging for both aesthetic and functional reasons. Many methods have been used for nasal reconstruction, for instance, dermal regeneration (intergra), skin grafts, and different kinds of skin flaps (frontal flap, frontonasal flap, nasolabial flap)1.
The nasolabial flap is one of the most commonly used methods for facial reconstruction surgeries2, with almost 100% survivability3. However, standard nasolabial flaps have some drawbacks, including a lack of proper curvature and difficulties to aesthetically blend with surrounding structures, especially in alar rim reconstructive surgeries4. There are also possible complications, such as trapdoor deformity or partial nostril collapse5. Other donor-site complications that have been reported including loss of nasolabial sulcal depth (8%) and subjective nasal obstruction (37%) without the use of cartilage grafts6.
In both primary and revision rhinoplasty, additional grafting materials, such as cartilage grafts, are required when there is a need for a stronger framework7.
Regarding cartilage graft selection, owing to the likelihood of causing dorsal irregularities and the lack of curvature compared to septal or rib cartilage, auricular cartilage is less preferred8. In such cases, rib cartilage can be combined with the nasolabial flap to reconstruct alar defects. However, since it is a type of hyaline cartilage, which is strong and stiff, it would be hard to remodel9.
We present a unique case involving remodification of an old costal cartilage graft, from an originally extended septal graft, into the right ala supportive frame. The combination of the nasolabial flap with this old graft might help with both the surface aesthetic and reforming the shape of the nasal ala. Similar research has yet to be done on this unusual case. We also observed the results from the procedure and the potential benefit of using costal versus auricular grafts in alar rim reconstructive surgeries.
Case Presentation
Patient History
A 33-year-old woman presented ten years ago with a primary nose infection that led to necrosis of the nasal tip and the entire right ala. She had an unremarkable medical, family, and psychosocial history.
The patient’s management at that time involved healing by secondary intention combined with antibiotic prophylaxis, followed by nasal reconstruction. At the first surgery, a medial arm flap and rib cartilage were used to reconstruct the nasal tip, right ala, and nasal dorsum. Flap division was complete after the pedicle was ligated three weeks after the operation.
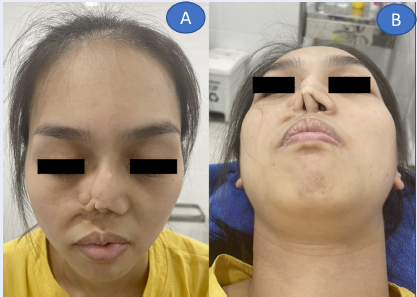
After a decade, the flap shrunk and became contractive, leading to reduced nostril opening and aesthetic defects. Although this insufficient reconstruction did not cause significant nasal blockage, it led to a lack of patient confidence in daily life (Figure 1).
| Timeline | Phase 1 | Phase 2 | |||
|---|---|---|---|---|---|
| Postoperative follow-up | |||||
| Admission/operating day (T0) | 3 days | 1 week | 3 weeks | 12–14 weeks | |
| Assessment/ Findings | + Contracture scarring, misshapen nose, and partial narrowing of the right nasal passage. + The old extended graft deviated rightward, causing alteration of the nasal height and loss of the right nasolabial fold. | Graft survived, no sign of infection. → Discharged | + Sutures removed. + Undergone healing process. + Appropriate shape of the nose. | Reassessment of reconstructive goals. | + Skin healing. + Assessment for second-phase aesthetic surgery. |
Clinical Findings and Diagnostic Assessment
Significant contracture scarring resulted in a misshapen nose and partial narrowing of the right nasal passage. The old extended graft deviated rightward, causing alteration of the nasal height and loss of the right nasolabial fold.
Prognosis
The patient’s nose had lost the right lateral crus, so a new cartilage graft was required to reshape the right alar rim.
Therapeutic Intervention — Surgical Procedure
The patient was later counseled at our clinic for a second nasal reconstructive surgery under local anesthesia, to which she agreed with written consent. Local anesthesia was selected because this was only a local modification surgery. The procedure used the old cartilage graft that was already in place and reshaping it to serve as a new alar rim without having to harvest new cartilage from another donor site. A two-phase surgical process was performed because there was not enough skin from the nasolabial graft to serve both of the above purposes in a single-phase surgery. The first phase of this surgery was mainly for reconstructive objectives to restore the patient’s right nasal structure.
The main incision was made from the tip of the nose in the columella region, along the patient’s old scar line until the base of the right nasal ala, exposing the underlying tissue. Throughout the process, bleeding was controlled with sterile gauze and bipolar electrocautery. A template was fashioned using a suture foil based on the unaffected left nasal ala, then reversed using a mirror image to transpose it to the right side. Exploration after wound excision showed only skin and scar tissues without any major alar cartilage left. For this reason, a cartilage graft was required.
Instead of harvesting new cartilage from another donor site, we reused the old 4-cm rib cartilage, which was initially used to increase the patient’s nasal height for aesthetic purposes. We trimmed and modified this old cartilage into a 2-cm graft based on the size of the proposed defect to fit into the alar lobule, reconstructing the right lateral crus of the alar cartilage. The graft was preserved in saline-soaked gauze for intermediate use. It would serve a new function as a framework to support the alar rim.
A right nasolabial flap was designed to fit the proposed area of skin replacement. The dissection for the flap goes deeper from distal to proximal toward the nasal base. Notably, we kept the subcutaneous fat layer intact.
After putting the cartilage graft in place, the flap was folded along the nasolabial fold, creating the newly reconstructed ala lining and the nasal tip. The lateral edges of the flap were sutured to the outer skin using Dafilon 6.0. Merocel (Hydroxylated Poly-Vinyl Acetate). Nasal packing was applied on the surgical area and fixed to the base of the columella to maintain the nasal opening. The dressing was done with petroleum-impregnated gauze.
Postoperative prophylactic management included: Amoxicillin + clavulanic acid1000 mg × 2 tablets/day, P.O for seven days; alpha chymotrypsin 21 ukatals× 2 tablets/day; P.O for five days, acetaminophen 500 mg × 3 tablets/day, P.O for five days.
The second phase will ideally be done after 12–14 weeks when the skin areas have healed and stabilized. This phase will focus on improving nasal aesthetics using a nanoform graft.
Postoperative Period and Timeline
There were concerns about the graft’s survivability due owing the purplish color of the distal area during the first several days post-operation. However, after the 3rd postoperative day, the flap survived and started healing, which signaled a successful surgery. The patient was discharged after the initial dressing and advised to follow up ten days later. The costal graft was appropriately in place without significant deviation. The graft’s survival depended on the diffusion of nutrients (Figure 1).
No other adverse events, such as infections or complications, were observed. The patient follow-up is divided into two main phases in this case. The first phase focused on the healing process and nasal reconstruction to ensure that there was no infection at the wound site and that the rib cartilage was in its correct position. The second phase will focus on flap survival and aesthetic improvement (Table 1).
Discussion
Nostril obstruction after flap repair of the ala reconstruction for carcinoma and trauma may be due to two factors. First, the bulky flap itself may obstruct the nostril. Second, the lack of support from the nasal cartilage structure allows the collapse of the ala to occur during inspiration under negative pressure10.
The nasolabial flap is a good choice for reconstructing alar defects, but it has some disadvantages, such as contracture scars, which can cause alar disfiguration11. In our report, a satisfactory aesthetic appearance cannot be achieved with this flap because it cannot enlarge and maintain the nostril’s shape; this finding is consistent with the findings of Arden & Miguel (2012) and Zhang, Yu, Song (2022), which require additional cartilage grafts to act as supportive structures6, 12.
Autologous rib cartilage can be combined with the nasolabial flap to reconstruct alar defects for several reasons. Firstly, it is an abundant source of cartilage with good biocompatibility, making it very versatile that has been well-described in the study by Fedok (2016); Rajbhandari, Kao (2016) and Won, Jin (2020)8, 13, 14. This accords with our earlier observation, which showed that the coastal graft provided a large amount of material for our procedure. Secondly, studies by Park, Jin (2012); Rajbhandari et al. (2019); Wee, Park, Oh, & Jin (2015); Won & Jin (2020) reported that if prevention and management protocols are followed correctly, there were relatively low rates of complications and morbidities, such as warping or infections. In our case, we adhered to the recommended postoperative management, which later showed improvements in graft survivability and no infection13, 14, 15, 16. Thirdly, costal cartilage has good stability for maintaining lateral crus structures and might also improve external nasal valve dysfunction (EVD) by increasing the cross-sectional area, which is great for aesthetic improvement17.
The advantage, in this case, is that the costal cartilage was already available on-site from previous surgery. After careful consideration of the need to harvest a new cartilage graft and the availability of an old one located nearby, which lost its previous function and caused nasal deformities, as well as surgical, anesthetic, satisfaction, and graft rejection risks18, we decided to use the old costal cartilage graft to create the framework for the alar rim. Limited research has been done on the application, effectiveness, and associated risks of modifying an old nasal graft for another function.
Conclusions
From our perspective, there are challenges in comparing and choosing between different grafting materials, such as ear, rib, or artificial cartilage in nasal alar reconstruction, nasal alar reconstruction still poses a challenge in need to compare different materials, such as ear, rib, or artificial cartilage. In our study, we believe that rib cartilage provides a more stable framework for both enlarging the airway and for aesthetic purposes. This result, optimistically, will encourage us to try more ways of approaching and application of artificial cartilage in future rhinoplasty surgeries.
Abbreviations
None.
Acknowledgments
None.
Author’s contributions
TVN and NTP proposed the idea and led the study. Other authors screened the paper, extracted the data, and wrote the manuscript. The study was conducted under the supervision of LTH and LHNM. All authors read and approved the final manuscript.
Funding
None.
Availability of data and materials
Data and materials used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Ethics approval and consent to participate
This study was conducted in accordance with the amended Declaration of Helsinki. This study was approved by the IRB of Plastic Surgery Korean Star Hospital (No: NCKH-2115), and all participants provided written informed consent.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
References
-
C.E. Montúfar,
V.A. Ugalde,
C.B. Kushida,
Reconstruction of Nasal Subunits using a Nasolabial Flap: Case Report. Journal of Surgery: Open Access.
2020;
7
(1)
:
dx.doi.org/10.16966/2470-0991.229
.
View Article Google Scholar -
Bayer
J.,
K. Schwarzmannová,
M. Dušková,
K. Novotná,
J. Kníže,
A. Sukop,
The nasolabial flap: the most versatile method in facial reconstruction. Acta Chir Plast.
2017;
59
(3-4)
:
135-41
.
-
Putri
I.L.,
W. Agustina,
M.R. Hutagalung,
Columella reconstruction using double nasolabial flap and costal cartilage: A case report. Annals of Medicine and Surgery.
2021;
64
:
102213
.
View Article PubMed Google Scholar -
Giles
W.C.,
C.W. Gross,
A.C. Abram,
W.M. Greene,
T.G. Avner,
How i do it head and neck and plastic surgery a targeted problem and its solution: Endoscopic septoplasty. The Laryngoscope.
1991;
104
(12)
:
1507-9
.
View Article Google Scholar -
H.C. Shim,
G. Kim,
J.H. Choi,
J.H. Kim,
E.J. Kim,
H.J. Park,
O.J. Joh,
S.J. Son,
The reverse nasolabial flap with a cartilage graft for the repair of a full-thickness alar defect: a single-stage procedure. Annals of Dermatology.
2014;
26
(3)
:
377-80
.
View Article PubMed Google Scholar -
Arden
R.L.,
Miguel
G.S.,
The subcutaneous melolabial island flap for nasal alar reconstruction: a clinical review with nuances in technique. The Laryngoscope.
2012;
122
(8)
:
1685-9
.
View Article PubMed Google Scholar -
Lee
L.N.,
Quatela
O.,
Bhattacharyya
N.,
The epidemiology of autologous tissue grafting in primary and revision rhinoplasty. The Laryngoscope.
2019;
129
(7)
:
1549-53
.
View Article PubMed Google Scholar -
Fedok
F.G.,
Costal cartilage grafts in rhinoplasty. Clinics in Plastic Surgery.
2016;
43
(1)
:
201-12
.
View Article PubMed Google Scholar -
Adams
C.,
Ratner
D.,
Composite and free cartilage grafting. Dermatologic clinics.
2005;
23
(1)
:
129-40
.
View Article PubMed Google Scholar -
Chait
L.A.,
Fayman
M.S.,
Treatment of postreconstructive collapsed nasal ala with a costal cartilage graft. Plastic and reconstructive surgery.
1988;
82
(3)
:
527-30
.
View Article PubMed Google Scholar -
Aksam
E.,
B. Aksam,
O. Karaaslan,
M.
Durgun,
Nasolabial flaps for nasal reconstruction: pros and cons. Turkish Journal of Plastic Surgery.
2018;
26
(4)
:
151
.
-
Zhang
Z.,
Z. Yu,
B. Song,
Septal extension graft for correcting short nose in East Asians: Review of autologous cartilage grafts and postoperative stability. British Journal of Oral and Maxillofacial Surgery.
2022;
60
(9)
:
1159-1165
.
View Article PubMed Google Scholar -
T.B. Won,
H.R. Jin,
Complications of costal cartilage Asian rhinoplasty and their management. Facial Plastic Surgery.
2020;
36
(5)
:
528-38
.
View Article PubMed Google Scholar -
Rajbhandari
S.,
Kao
C.H.,
Research
A.,
Costal cartilage graft in Asian rhinoplasty: surgical techniques. Plastic and Aesthetic Research.
2019;
6
:
8
.
View Article Google Scholar -
Park
J.H.,
Jin
H.R.,
Use of autologous costal cartilage in Asian rhinoplasty. Plastic and reconstructive surgery.
2012;
130
(6)
:
1338-48
.
View Article PubMed Google Scholar -
Wee
J.H.,
M.H. Park,
S. Oh,
H.R. Jin,
Complications associated with autologous rib cartilage use in rhinoplasty: a meta-analysis. JAMA facial plastic surgery.
2015;
17
(1)
:
49-55
.
View Article PubMed Google Scholar -
Taha
M.A.,
C.A. Hall,
H.E. Zylicz,
W.T. Barham,
M.B. Westbrook,
M.J. Barham,
M.M. Stevenson,
B.A. Zito,
H.P. Barham,
Costal Cartilage Lateral Crural Strut Graft for Correction of External Nasal Valve Dysfunction in Primary and Revision Rhinoplasty. Ear, Nose & Throat Journal.
2021;
2021
:
0145561320983940
.
View Article PubMed Google Scholar -
Wee
J.H.,
S.J. Mun,
W.S. Na,
H. Kim,
J.H. Park,
D.K. Kim,
H.R. Jin,
Autologous vs irradiated homologous costal cartilage as graft material in rhinoplasty.. JAMA facial plastic surgery.
2017;
19
(3)
:
183-8
.
View Article Google Scholar
Comments
Article Details
Volume & Issue : Vol 10 No 3 (2023)
Page No.: 5609-5613
Published on: 2023-03-31
Citations
Copyrights & License

This work is licensed under a Creative Commons Attribution 4.0 International License.
Search Panel
- HTML viewed - 5169 times
- PDF downloaded - 1242 times
- XML downloaded - 130 times
 Biomedpress
Biomedpress



