
A revolution in the treatment of aggressive liposarcoma by pazopanib combined with chemotherapy- A case report
- Medical Biology Research Center, Kermanshah University of Medical Sciences, Kermanshah, Iran
- Department of Hematology, Shahid Beheshti University of Medical Sciences, Tehran, Iran
- Department of Hematology, Iran University of Medical Science, Tehran, Iran
- Department of Genetics, Shahid Sadoughi University of Medical Sciences, Yazd, Iran
Abstract
Pazopanib is a new tyrosine kinase inhibitor which acts as anti-VEGF signaling and antiangiogenesis. In some countries, this drug has been approved for the treatment of advanced, or metastatic soft tissue sarcoma. Nevertheless, the efficacy of Pazopanib has not yet been proven in patients with advanced liposarcoma. We reported a rare case of advanced liposarcoma that after several courses of chemotherapy, the disease was relapsed, and CT-scan results showed lung metastasis. Therapeutic measures, including surgery and chemotherapy with pazopanib, were successful in destroying the metastatic mass in the patient's lung. Our finding provides a new therapeutic approach for pleomorphic liposarcoma.
Introduction
Liposarcoma (LPS) represents the most common soft tissue sarcoma (STS) 1. This malignancy engages adipocyte tissue that is present in 12.8% of all sarcomas 2. The proportion of STS of all malignancies is 1% in adults 3. LPS is seen in 45% of retroperitoneal tumors and 24% of limb tumors 4. The growth rate of the tumor is low, and this malignancy has few symptoms, including a retroperitoneum lesion that can quickly develop 5. LPS is characterized by noticeable mortality and morbidity. The poor prognosis of LPS depends on the histological pattern, the organ of origin, and the location where malignancy arises and tumor originate 6. Therapeutic strategy for patients with LPS includes chemotherapy, radiation therapy, surgical and tissue sparing. However, the complete treatment of LPS is a challenge 6,7. Therefore, a new strategy is required for a more effective treatment. The purpose of this paper is to report a case of a 35-year-old man with advanced liposarcoma, who were treated with pazopanib.
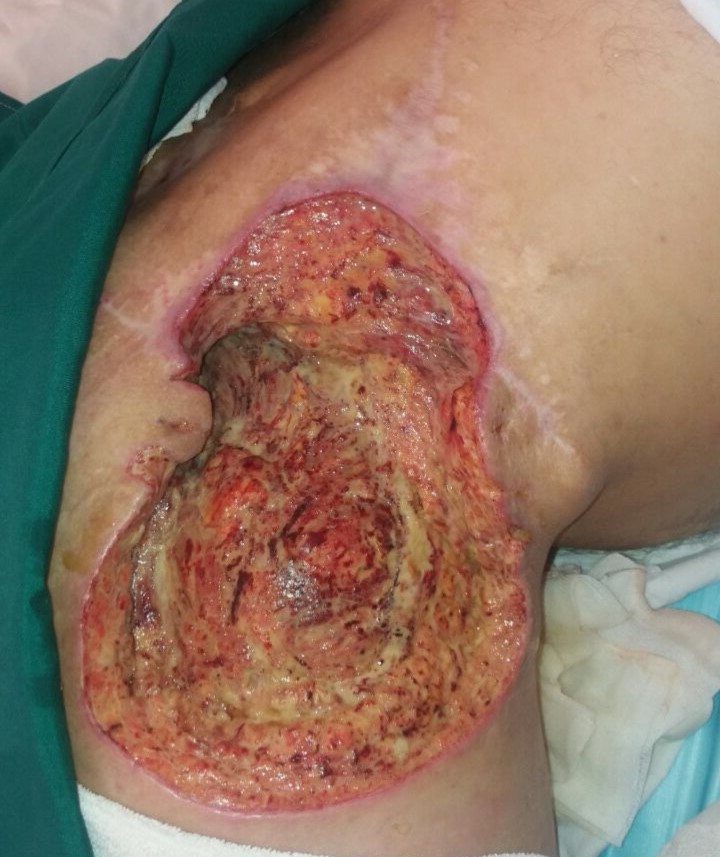
Fatty lesions in right gluteal tissue.

Surgical resection for lesions removal.
CASE PRESENTATION
In February 2017, a 35-year-old man was referred to the Clinic of Hematology and Oncology, with painful scar history and swelling in the left pelvis (Figure 1). After a physical examination of the patient, the physician asked for a CT scan and a biopsy from the pelvis. The pathology report showed a hypodense lesion with a diameter of more than 10 x 3 cm in the right gluteal tissue. Also, the results of IHC were as follows: S100 and Ki67 were positive, and Desmin, CD99, and CK were negative. According to these results, the disease was diagnosed as a high-grade pleomorphic liposarcoma with stage III development. Therefore, treatments such as radiotherapy (30 sessions) and surgery in the gluteal region were performed, and the lesion removed (Figure 2). Following the surgery, the combination of chemotherapy with Doxorubicin and Ifosfamide was administered for six courses. During the treatment, blood test and kidney function tests were normal. After completing this course, the patient's condition was satisfactory, and the progress of the disease was terminated. In August 2018, the patient referred to the clinic again with symptoms such as pain of the pelvic regions and problems with breathing. CT scan of the chest was performed to examine the status of the lungs, which showed multiple nodules in the right lower lobe of the lung. This was diagnosed as a metastatic tumor (Figure 3). Also, gluteal lesion biopsy showed local recurrence in this area. The patient was treated by chemotherapy with Pazopanib (200 mg), Eribulin, and Dacarbazine for ten sessions. As the lesion was shrunk, it was removed by a surgical procedure, and treatment was continued with pazopanib. Pulmonary CT scan revealed no sign of pulmonary nodules (Figure 4). The patient is currently in good condition and is under follow-up.
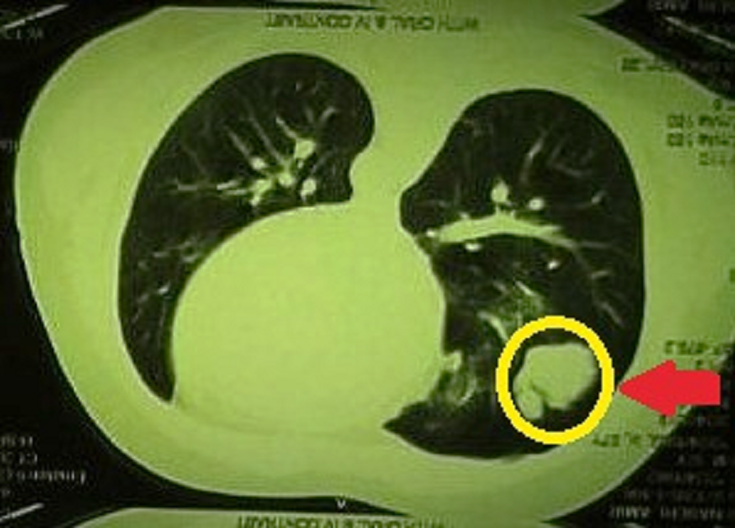
Metastatic nodules in the right lower lobe of the lung.
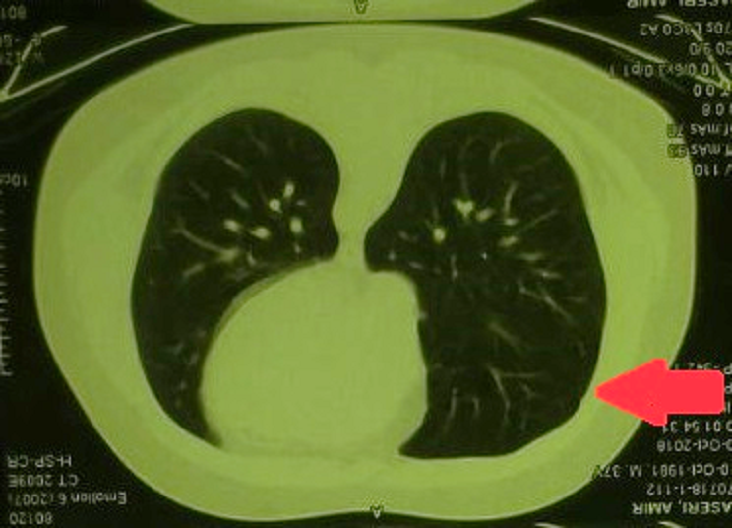
Disappeared pulmonary nodules after treatment with Pazopanib.
DISCUSSION
Liposarcoma is a subgroup of STS, which arises from adipocyte tissue, and its metastasis is seen in 35% of cases8. LPS is classified into five categories according to the histological characteristics: Well Differentiated (WDLS), Dedifferentiated (DDLS), Myxoid (MLS), Round (RLS) and Pleomorphic (PLPS). WDLS and DDLS are the most common types of LPS (more than 60%) 9. Complex karyotype of PLPS has been shown to cause disruption in the activity of tumor suppressor genes, P53, and Rb. The incidence of this type is rare (nearly 5%), and its characteristic is poorly diagnosed9,10. For localized LPS, surgical resection is an effective treatment, but there is a debate about the application of radiation and common cytotoxic therapy for metastatic and unresectable STS. Thus, there is a requirement for a new approach and targeted therapy 11. Indeed, the recurrence of the disease after surgery is common, and the overall 5-year survival is low (about 65%). Radiation therapy and conventional chemotherapy can be useful to reduce local and distant recurrence; however, each of them has limitations such as significant toxicity, poor tolerability, and limited efficacy 12.
The first line of treatment for STS is the use of cytotoxic chemotherapy agents such as Anthracycline base (predominantly doxorubicin), Gemcitabine base, Dacarbazine, and Ifosfamide. Combined therapy (doxorubicin with ifosfamide) is preferred for monotherapy, due to increased response rates and disease control, but has no potential effect on the overall survival 13,14,15. The second line of treatment comprises of Ifosfamide, Dacarbazine, Trabectin, and pazopanib, which are selected based on poor response to treatments, low progression-free survival (PFS) and OS. The efficacy of these drugs in STS is not satisfactory16,17. Therefore, better approaches and more effective agents are required for advanced STS.
In LPS, the expression of tyrosine kinase receptors such as MET, AXL, IGFR, EGFR is increased. Thus, targeted therapy by inhibition of these factors is appropriate for LPS treatment. An instance of tyrosine kinase inhibitors (TKI) is pazopanib, which is a synthetic indazolyl pyrimidine and targets VEGFR, PDGFR, and C-kit 11.
Preclinical studies to assess pazopanib in LPS indicated that this drug had an impressive role in reducing the proliferation of tumor cells and preventing angiogenesis 18. In our case, the patient underwent surgery and treatment with chemotherapy agents such as Ifosfamide, and Adriamycin for six months. However, after this period, local recurrence and lung metastasis were observed. Therefore, the new regimen therapy with eribulin and dacarbazine was initiated along with pazopanib. Following treatment with pazopanib, lung metastasis was eradicated, and the lesion was reduced.
CONCLUSION
Due to the high rate of metastasis in pleomorphic liposarcoma, the effectiveness of chemotherapy as the only treatment option is still debatable. Therefore, treatment in this type of liposarcoma is challenging. The use of new therapies, such as tyrosine kinase inhibitors (pazopanib) can be effective in treating this disease.
Abbreviations
EGFR: Epidermal growth factorLPS: liposarcoma
IGFR: Insulin-like growth factor receptorOS: overall survival
PDGFR: Platelete-drived growth factor receptor
PFS: progression- free survival
STS: soft tissue sarcoma
TKI: tyrosine kinase inhibitor
VEGFR: Vascular endothelial growth factor
Competing Interests
The authors declare that they have no financial or other conflicts of interest.
Authors' Contributions
Mehrdad Payandeh & Afshin Karami: Literature search, Clinical studies, Data acquisition, Data analysis; Afshin Karami: Manuscript preparation, Manuscript review, Guarantor; Noorodin Karami: Concepts, Design, Definition of intellectual content, Literature search, Manuscript editing; Samira Rahimi, & Mehrnoush Aeinfar: Manuscript editing, Manuscript preparation, Literature search. All authors read and approved the final manuscript.

