Abstract
Background: Vomiting occurs when the contractions of stomach muscle walls cause a large amount of the stomach content to go upward and flow back into the esophagus; this process is very common among infants. The aim of this review was to present the effects of medicinal plants on vomiting.
Methods: In the current review, articles indexed in databases such as ISI, PubMed, Scopus, Islamic World Science Citation Center, Scientific Information Database, and Magiran were retrieved using the search terms ‘vomiting’, ‘nausea’, ‘medicinal plants’, and ‘traditional medicine’.
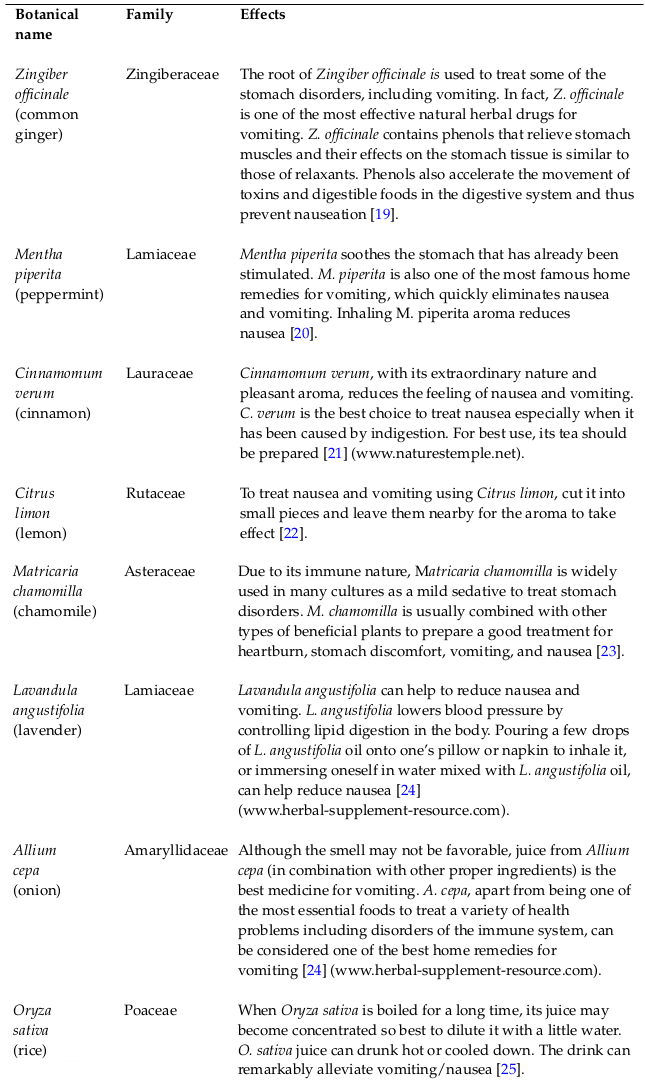
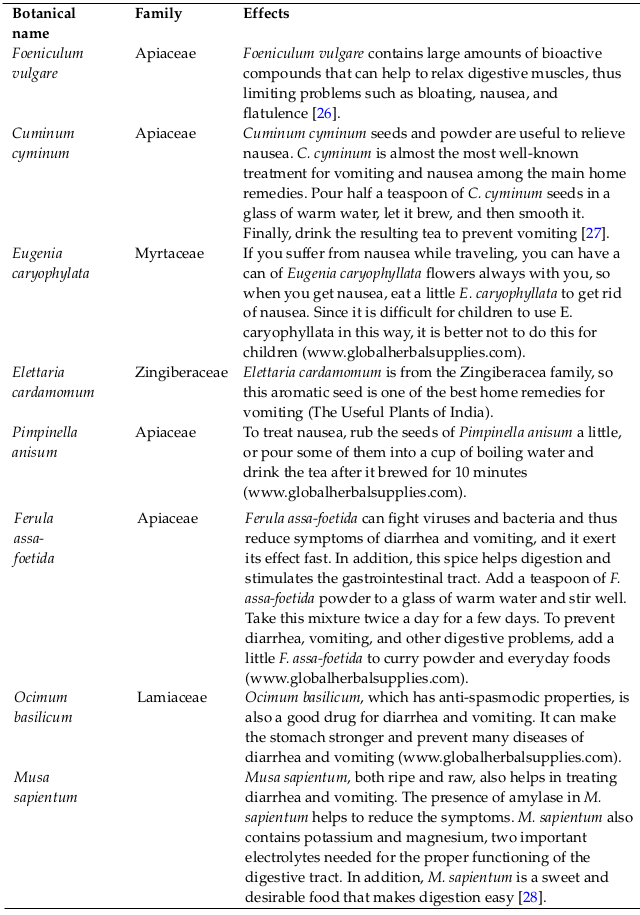
Results: Based on the research findings, the medicinal plants Zingiber officinale, Mentha piperita, Cinnamomum verum, Citrus limon, Matricaria chamomilla, Lavandula angustifolia, Allium cepa, Oryza sativa, Foeniculum vulgare, Cuminum cyminum, Eugenia caryophyllata, Elettaria cardamomum, Pimpinella anisum, Ferula assa-foetida, Ocimum basilicum, and Musa sapientum were selected as the focus.
Conclusion: In traditional medicine, treatment for vomiting is relevant, especially in children. The mechanisms of some of these plants have been understood but for many they are still unclear. Further investigations are needed to understand more about these medicinal plants and their mechanism of action for effective use in the clinic.
Introduction
Vomiting occurs when the contractions of stomach muscle walls cause a large amount of stomach contents to push upward and flow back into the esophagus, exiting through the mouth (or nose). Since the food is traveling upward, some of the foods and liquids will involuntarily flow back into the mouth [1]-[3]. Vomiting or spitting up food is very common among infants and not too worrying of an issue. However, vomiting can be dangerous if it causes loss of a lot of fluids, leading to dehydration in the baby [2]-[4]. If the baby vomits immediately after eating, it may reflect a more serious problem. Reflux occurs when the muscles between the esophagus and the stomach do not work properly and thus the contents of the stomach flow back into the pharynx [5]. Vomiting can be caused many various factors, including viral or bacterial infection, stomach infections, urinary tract infections, pneumonia, meningitis, strep throat, and even ear infections. Crying, toxic substances, and intestinal obstruction are also other factors which may cause vomiting [4][5].
In spite of significant progress in the prevention and treatment of nausea and vomiting, their effective management is still a major problem. It should be noted that severe vomiting can lead to development of many complications, such as dehydration, weight loss, fluid- electrolyte imbalance, anorexia, esophageal tears, weakness, wound dehiscence, fractures, pre- renal azotemia, or decline in behavioral and mental status [6]. The adverse effects of vomiting can deteriorate the patient’s self-care, physical and mental status, as well as functional abilities. This can increase the patient’s anxiety and dissatisfaction with the hospital experience, which in turn can contribute to future anticipatory nausea [7].
Prevention and treatment of vomiting by safe remedies are, therefore, essential. Complementary therapies have been widely used worldwide; moreC than 80% of the world’s population rely on complementary and alternative therapies for their health care [8]-[10]. Currently, people all over the world, especially in developing countries, pay attention to medicinal plants [11]-[14]. These plants have been shown to be reliable in the treatment of various diseases as well as in the preparation of new medicines [15][16]. The active ingredients of these herbal remedies (drugs) are being extensively investigated due to the popularity and acceptance of herbal remedies [14][17].
In this regard, medicinal plants have been mostly used in various traditional systems and have been in use for a long time [9][18]. Traditional knowledge on the use of medicinal plants have contributed to the development of antiemetic remedies. Since the prevalence of vomiting in infants and children is high, in this review, traditional medicine and phyto-medicine for vomiting are investigated; the study herein evaluates how herbal remedies affect vomiting in children.
Materials and Methods
In the current review, articles were indexed from certain databases, including ISI, PubMed, Scopus, Islamic World Science Citation Center, Scientific Information Database, and Magiran. They were retrieved by using the search terms ‘vomiting’, ‘nausea’, ‘ulcer’, ‘medicinal plants’, and ‘traditional medicine’.
Results
Based on the search, the results showed that several plants are used in traditional medicine to treat vomiting in all people, especially children. The following are the medicinal plants: Zingiber officinale, Mentha piperita, Cinnamomum verum, Citrus limon, Matricaria chamomilla, Lavandula angustifolia, Allium cepa, Oryza sativa, Foeniculum vulgare, Cuminum cyminum, Eugenia caryophyllata, Elettaria cardamomum, Pimpinella anisum, Ferula assa-foetida, Ocimum basilicum, and Musa sapientum Table 1 and Table 2 .
Discussion
In this review article, medicinal plants used against vomiting are reported. Traditional knowledge of these plants can contribute to development of antiemetic remedies. Chronic nausea is usually multifactorial in origin. High intracranial pressure, dehydration, gastroduodenal ulcers, bowel obstruction, and metabolic abnormalities (including uremia, hyponatremia and hypercalcemia) can contribute to nausea and vomiting. Psychological parameters also can induce or exacerbate it [29]. Vomiting and nausea both are mediated and controlled through central nervous system, however, by different mechanisms. Vomiting is mediated through stimulation of a complex reflex which is coordinated through a putative true vomiting center; nausea, however, results from the stimulation of autonomic nervous system.
The vomiting center usually receives afferent stimuli through various central neurologic pathways. For example, various sensory stimuli of psychological response (e.g. taste, smell, and pain) from the limbic system are able to stimulate the chemoreceptor trigger zone (CTZ) and cause vomiting. Motion sickness, however, occurs through impulses from the labyrinthine apparatus. Endogenous biochemical and exogenous substances which accumulate during irritation, ischemia and inflammation can stimulate spinal and vagal nerves to cause nausea and vomiting. Intestinal damage or irritation also cause substantial generation and release of serotonin by the enterochromaffin cells in the enteric nervous system of serotonin, which stimulates 5HT3 receptors and causes severe vomiting [30]. The central pathway is also stimulated by substance P, which in turn stimulates the neurokinin-1 receptors and the gastrointestinal vagal afferent nerve fibers. Several other receptors such as CB1 (canabinoid-1), H1 (histamine-1), D2 (dopamine-2), D3 (dopamine-3), M3 (muscarinic-3), M5 (muscarinic-5), and GABAB (gamma amino butyric acid-B) contribute to vomiting [30][31]. Thus, medicinal plants with antiemetic activities can act through various pathways. The mechanisms of action of these plants should be investigated; the modes of actions of only some of these plants have been studied so far.
Studies have also suggested the association of oxidative stress and clinical severity of vomiting and nausea [32]. This is an important issue in the use of medicinal plants as antiemetic agents. Plants, including the medicinal plants presented in this review article, mostly have antioxidant activity [33]–[35]. Antioxidants can scavenge the free radicals and return the imbalance between antioxidant activity and oxidative stress, which are induced by various diseases [13][36][37]. Therefore, each medicinal plant should be studied not only for their mode of action but also for their ability to reduce oxidative stress. Furthermore, each medicinal plant may have its own effects on a wide range of diseases [38]-[41]. Therefore, these herbal remedies may benefit the patient (adult or child) in treating emesis as well as other diseases. Moreover, the use of these herbal remedies would be associated with lower cost and greater safety than non-herbal remedies.
Conclusion
Although the mechanisms of action for some of these plants have been understood, there are many other plants (reviewed in this article) whereby the mechanism of action has not been elucidated. All the plants discussed in this article are beneficial against vomiting and nausea. However, future investigations are needed to explore the most effective of these medicinal plants for use in treating nausea/vomiting in the clinic.
Open Access
This article is distributed under the terms of the Creative Commons Attribution License (CC-BY 4.0) which permits any use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited.
List of abbreviations
Vom: Vomiting, Nau: nausea
Competing interests
The authors declare that they have no conflict of interest
Funding
There is no financial support for this study
Authors’ contributions
All authors reviewed, commented and approved the final manuscript.
References
-
GM
Walker,
A
Neilson,
D
Young,
PA
Raine.
Colour of bile vomiting in intestinal obstruction in the newborn: questionnaire study. Bmj.
2006;
332
:
1363
.
View Article Google Scholar -
HH
Pomerance.
Nelson textbook of pediatrics. Archives of pediatrics & adolescent medicine.
1997;
151
:
324-324
.
View Article PubMed Google Scholar -
D
Marlow.
Textbook of pediatric nursing. In Textbook of pediatric nursing Philadelphia. Saunders.
1969
.
-
GR
Fleisher,
S
Ludwig.
Textbook of pediatric emergency medicine. Lippincott Williams & Wilkins.
2010
.
-
MC
Rogers.
Textbook of pediatric intensive care. Lippincott Williams and Wilkins.
1992
.
-
ES
Antonarakis,
RDW
Hain.
Nausea and vomiting associated with cancer chemotherapy: drug management in theory and in practice. Archives of disease in childhood.
2004;
89
:
877-880
.
View Article PubMed PMC Google Scholar -
HJ
Thompson.
The management of post-operative nausea and vomiting. Journal of advanced nursing.
1999;
29
:
1130-1136
.
View Article PubMed Google Scholar -
F
Jamshidi-Kia,
Z
Lorigooini,
H
Amini-Khoei.
Medicinal plants: past history and future perspective. Journal of herbmed pharmacology.
2018;
1
:
1-7
.
-
RD
Sewell,
M
Rafieian-Kopaei.
The history and ups and downs of herbal medicines usage. Journal of Herbmed Pharmacology.
2014;
3
.
-
H
Nasri,
H
Shirzad.
Toxicity and safety of medicinal plants. Journal of HerbMed Pharmacology.
2013;
2
.
-
S
Asgari,
M
Setorki,
M
Rafieian-kopaei,
N
Shahinfard,
R
Ansari,
al
Forouz Z et.
Postprandial hypolipidemic and hypoglycemic effects of Allium hertifolium and Sesamum indicum on hypercholesterolemic rabbits. African Journal of Pharmacy and Pharmacology.
2012;
6
:
1131-1135
.
-
L
Jalaly,
G
Sharifi,
M
Faramarzi,
A
Nematollahi,
M
Rafieian-Kopaei,
M
Amiri,
F
Moattar.
Comparison of the effects of Crataegus oxyacantha extract, aerobic exercise and their combination on the serum levels of ICAM-1 and E-Selectin in patients with stable angina pectoris. DARU Journal of Pharmaceutical Sciences.
2015;
23
:
54
.
View Article PubMed PMC Google Scholar -
E
Shayganni,
M
Bahmani,
S
Asgary,
M
Rafieian-Kopaei.
Inflammaging and cardiovascular disease: Management by medicinal plants. Phytomedicine.
2016;
23
:
1119-1126
.
View Article PubMed Google Scholar -
M
Rahimi-Madiseh,
E
Heidarian,
S
Kheiri,
M
Rafieian-Kopaei.
Effect of hydroalcoholic Allium ampeloprasum extract on oxidative stress, diabetes mellitus and dyslipidemia in alloxan-induced diabetic rats. Biomedicine & Pharmacotherapy.
2017;
86
:
363-367
.
View Article PubMed Google Scholar -
Z
Rabiei,
M
Gholami,
M
Rafieian-Kopaei.
Antidepressant effects of Mentha pulegium in mice. Bangladesh Journal of Pharmacology.
2016;
11
:
711-715
.
View Article Google Scholar -
M
Asadi-Samani,
N
Bagheri,
M
Rafieian-Kopaei,
H
Shirzad.
Inhibition of Th1 and Th17 cells by medicinal plants and their derivatives: A systematic review. Phytotherapy Research.
2017
.
View Article PubMed Google Scholar -
M
Rahimi-Madiseh,
P
Karimian,
M
Kafeshani,
M
Rafieian-Kopaei.
The effects of ethanol extract of Berberis vulgaris fruit on histopathological changes and biochemical markers of the liver damage in diabetic rats. Iranian journal of basic medical sciences.
2017;
20
:
552
.
PubMed PMC Google Scholar -
F
Jamshidi-Kia,
Z
Lorigooini,
H
Amini-Khoei.
Medicinal plants: past history and future perspective. Journal of herbmed pharmacology.
2018;
1
:
1-7
.
-
WM
Marx,
L
Teleni,
AL
McCarthy,
L
Vitetta,
D
McKavanagh,
D
Thomson,
E
Isenring.
Ginger (Zingiber officinale) and chemotherapy-induced nausea and vomiting: a systematic literature review. Nutrition reviews.
2013;
71
:
245-254
.
View Article PubMed Google Scholar -
Z
Tayarani-Najaran,
E
Talasaz-Firoozi,
R
Nasiri,
N
Jalali,
MK
Hassanzadeh.
Antiemetic activity of volatile oil from Mentha spicata and Mentha piperita in chemotherapy - induced nausea and vomiting. ecancermedicalscience.
2013;
7
.
-
null
null.
http://www.naturestemple.net/cinnamon-cinnamomum-verum/.
.
-
F
Safajou,
M
Shahnazi,
al
Nazemiyeh H et.
The effect of lemon inhalation aromatherapy on nausea and vomiting of pregnancy: a double-blinded, randomized, controlled clinical trial. Iranian Red Crescent Medical Journal.
2014;
16
.
-
F
Sanaati,
S
Najafi,
Z
Kashaninia,
M
Sadeghi.
Effect of ginger and chamomile on nausea and vomiting caused by chemotherapy in iranian women with breast cancer. Asian Pac J Cancer Prev.
2016;
17
:
4125-9
.
PubMed Google Scholar -
null
null.
https://www.herbal-supplement-resource.com/lavender-oil.html.
.
-
M
Umadevi,
R
Pushpa,
KP
Sampathkumar,
D
Bhowmik.
Rice-traditional medicinal plant in India. Journal of pharmacognosy and phytochemistry.
2012;
1
.
-
H
Pasha,
F
Behmanesh,
F
Mohsenzadeh,
M
Hajahmadi,
AA
Moghadamnia.
Study of the effect of mint oil on nausea and vomiting during pregnancy. Iranian Red Crescent Medical Journal.
2012;
14
:
727
.
View Article PubMed PMC Google Scholar -
M
Rahimi-Madiseh,
Z
Lorigoini,
H
Zamani-gharaghoshi,
M
Rafieian-kopaei.
Berberis vulgaris: specifications and traditional uses. Iranian journal of basic medical sciences.
2017;
20
:
569
.
PubMed PMC Google Scholar -
SS
Dahham,
TA
Mohamad,
YM
Tabana,
A
Majid.
Antioxidant activities and anticancer screening of extracts from banana fruit (Musa sapientum). Academic J Cancer Res.
2015;
8
:
28-34
.
-
A
Berger,
R
Clark-Snow.
Nausea and vomiting. In Jr DV, S H, SA R, editors, Cancer: Principles and Practice of Oncology pp. 2705-2712 Philadelphia, PA. Lippincott Raven.
1997
.
-
RK
Portenoy,
AM
Berger,
DE
Weissman.
Principles and practice of supportive oncology. Lippincott-Raven.
1998
.
-
P
Pasricha.
Treatment of disorders of bowel motility and water flux; antiemetics; agents used in biliary and pancreatic diseases. In Ll B, Js L, Kl P, editors. Goodman and Gilman's The Pharmacological Basis of Therapeutics pp. 983-1008 New York, NY. McGraw-Hill.
2005
.
-
F
Verit,
O
Erel,
M
Sav,
N
Celik,
D
Cadirci.
Oxidative stress is associated with clinical severity of nausea and vomiting of pregnancy. Am J Perinatol.
2007;
24
:
545-548
.
View Article PubMed Google Scholar -
H
Shirzad,
M
Shahrani,
M
Rafieian-Kopaei.
Comparison of morphine and tramadol effects on phagocytic activity of mice peritoneal phagocytes in vivo. International immunopharmacology.
2009;
9
:
968-970
.
View Article PubMed Google Scholar -
S
Asgharzade,
M
Rafieian-kopaei,
A
Mirzaeian,
S
Reiisi,
L
Salimzadeh.
Aloe vera toxic effects: expression of inducible nitric oxide synthase (iNOS) in testis of Wistar rat. Iranian journal of basic medical sciences.
2015;
18
:
967
.
PubMed PMC Google Scholar -
Z
Rabiei,
S
Naderi,
M
Rafieian-Kopaei.
Study of antidepressant effects of grape seed oil in male mice using tail suspension and forced swim tests. Bangladesh Journal of Pharmacology.
2017;
12
:
397-402
.
View Article Google Scholar -
H
Rouhi-Boroujeni,
E
Heidarian,
H
Rouhi-Boroujeni,
F
Deris,
M
Rafieian-Kopaei.
Medicinal plants with multiple effects on cardiovascular diseases: A systematic review. Current pharmaceutical design.
2017;
23
:
999-1015
.
View Article PubMed Google Scholar -
Z
Rabiei,
M
Rafieian-Kopaei,
S
Mokhtari,
M
Shahrani.
Effect of dietary ethanolic extract of Lavandula officinalis on serum lipids profile in rats. Iranian journal of pharmaceutical research: IJPR.
2014;
13
:
1295
.
PubMed PMC Google Scholar -
A
Karimi,
M
Mohammadi-Kamalabadi,
M
Rafieian-Kopaei,
L
Amjad.
Determination of antioxidant activity, phenolic contents and antiviral potential of methanol extract of Euphorbia spinidens Bornm (Euphorbiaceae). Tropical Journal of Pharmaceutical Research.
2016;
15
:
759-764
.
View Article Google Scholar -
Z
Hosseini,
Z
Lorigooini,
M
Rafieian-Kopaei,
HA
Shirmardi,
K
Solati.
A review of botany and pharmacological effect and chemical composition of Echinophora species growing in Iran. Pharmacognosy research.
2017;
9
:
305
.
View Article PubMed PMC Google Scholar -
E
Heidarian,
M
Rafieian-Kopaei.
Protective effect of artichoke (Cynara scolymus) leaf extract against lead toxicity in rat. Pharmaceutical biology.
2013;
51
:
1104-1109
.
View Article PubMed Google Scholar -
A
Baradaran,
H
Nasri,
M
Rafieian-Kopaei.
Erythropoietin and renal protection. DARU Journal of Pharmaceutical Science.
2013;
21
:
78
.
View Article PubMed PMC Google Scholar
Comments

Downloads
Article Details
Volume & Issue : Vol 5 No 5 (2018)
Page No.: 2252-2259
Published on: 2018-05-11
Citations
Copyrights & License

This work is licensed under a Creative Commons Attribution 4.0 International License.
Search Panel
Pubmed
Google Scholar
Pubmed
Google Scholar
Pubmed
Google Scholar
Pubmed
Search for this article in:
Google Scholar
Researchgate
- HTML viewed - 15163 times
- Download PDF downloaded - 3670 times
- View Article downloaded - 0 times
 Biomedpress
Biomedpress